Healthcare workers can come across a wide array of occupational hazards on the job. When working with sick and infected patients, it is only natural to come into contact with various fluids and dangerous materials, including blood. To ensure patient and worker safety, having the right personal protective equipment, or PPE for bloodborne pathogens, is crucial to prevent the contact and spread of potential diseases.
This article outlines the various dangers that healthcare workers can face on the job and how having high-quality PPE can make these environments safer for everyone involved.
What is a Bloodborne Pathogen?
According to the Center for Disease Control, a bloodborne pathogen is a microorganism that can pass through the bloodstream. For these pathogens to transfer from person to person, they have to enter both individuals' bloodstream. The most common transmission method of bloodborne pathogens is through open wounds, such as a small cut.
The most common examples of bloodborne pathogens include:
- Hepatitis B Virus (HBV)
- Human Immunodeficiency Virus (HIV)
- Hepatitis C Virus (HCV)
The CDC estimates that roughly 5.6 million healthcare workers are regularly exposed to these pathogens and other potentially infectious materials (OPIM). OPIM can include other bodily fluids, such as saliva, cerebrospinal fluid, amniotic fluid, and others.
What Type of Exposure to Bloodborne Pathogens Requires PPE?
Because healthcare workers can be exposed to blood and other bodily fluids in multiple situations, employers must provide sufficient personal protective equipment for their safety. The amount of PPE and exposure level can vary depending on the environment and circumstances.
For example, if a lab technician is drawing blood, wearing disposable gloves should be sufficient to prevent any accidental transmission. However, in situations where blood may be more prevalent (i.e., during an autopsy), more equipment may be required, such as gowns, face shields, masks, and eye protection. The more likely that blood is to spray or splatter, the more protection workers need to stay safe.
Simply put, if a healthcare worker is going to be in a situation where blood or OPIM may be present, sufficient PPE must be provided.
What are OSHA and CDC Recommendations for Working with Bloodborne Pathogens?
Both the Occupational Health and Safety Administration (OSHA) and CDC have various standards for working with bloodborne pathogens known as the BBP standard. These regulations are designed to protect both workers and patients, and it is up to the employer to provide sufficient protective materials for all employees. Here is a breakdown of the core elements of the BBP standard:
- Universal Precautions (UP) - This standard was introduced in the 1980s, and the idea is to treat all instances of blood and other bodily fluids as infectious. If workers assume that a sample is contaminated, they are far more likely to take the threat seriously.
- Standard Precautions (SP) - While UP standards provided a cautious work environment, they didn't outline specific containment methods and cleanup of blood and OPIM. In 1996, additional standard precautions were introduced. These components included rules regarding hand washing, personal hygiene, safe injection practices when handling needles, the presence of PPE in the workplace based on anticipated needs, and more. By utilizing these precautions, healthcare workers can be much more proactive about protecting themselves and their patients.
- Transmission-Based Precautions (TBP) - Although standard and universal precautions provide guidelines in the workplace, TBP goes a step further and addresses specific instances where transmission may be likely. For example, if blood sprays or droplets get into the air or onto surfaces, workers are trained on how to clean up the contamination without risk to themselves or the patient.
Although these standards are used for bloodborne pathogens, they also apply to all bodily fluids, including vomit, urine, saliva, and others. Again, it is up to the employer to provide the right PPE and training for workers to follow these guidelines, as necessary.
What PPE is Recommended When Working With Bloodborne Pathogens?
While work environments vary, there are numerous types of personal protective equipment that can help prevent the spread of bloodborne pathogens. Depending on the situation, employers must provide any, or all, of the following pieces to protect workers and patients.
- Disposable Gloves
- Full Face Shield
- Eye Goggles
- Face Masks
- Safety Glasses With Side Shields
- Aprons
- Lab Coats
- Protective Apparel
- Gowns
- Mouthpieces for Resuscitation
- Bloodborne Pathogen Kits Filled with Protective Items
In all cases, PPE for healthcare workers must not allow for the transmission of fluids. In instances where needles and other sharp objects are used, employers must provide extra equipment to ensure that nothing can penetrate the skin by accident. For example, workers may use thicker gloves and additional barriers when working with needles, such as a protective face shield.
What is the Process for Decontamination and Disposal of This PPE?
To prevent cross-contamination after the fact, all PPE must either be decontaminated or disposed of properly after each use. Typically, equipment is designed for single-use purposes, such as disposable aprons, gloves, and gowns. Sturdier materials like face shields and goggles may be cleaned and reused. Here is a rundown of OSHA and CDC guidelines regarding PPE decontamination and disposal.
- Marked Bins - All PPE must be placed in appropriately sealed containers. Materials that will be discarded must be separated from those that will be cleaned or reused. If any component is damaged, cracked, or worn, it must be disposed of correctly.
- Cleaning - In instances where blood and other fluids are present, workers must clean them as quickly as possible using CDC-approved disinfectants and cleaners. It is recommended to use tongs and other devices to avoid direct contact, even if the worker is wearing gloves. The CDC warns against using aerosols and sprays that could spread pathogens by turning them into droplets in the air.
- Disposal - All PPE should be bagged and placed in leak-proof containers, whether they are contaminated or not. Needles and other sharp objects must be placed in a corresponding safety bin to ensure that they will not pose a potential hazard.
- Removal of PPE - The CDC recommends that workers remove any covering in this order: gloves, face shield/goggles, gown/apron, face mask. Once all pieces are removed, workers must wash their hands thoroughly to prevent any potential cross-contamination.
What are ASTM 1670 and ASTM 1671 Tests? Why Are These Tests Important?
Because transmission of bloodborne pathogens is so serious, there must be standards to ensure that all PPE for bloodborne pathogens will protect workers in all situations. In the U.S., there are two primary tests available for PPE - ASTM 1670 (Blood) and ASTM 1671 (Bloodborne Pathogens). Here is a breakdown of both trials and how they are implemented.
- ASTM 1670 - This test aims to see whether synthetic blood can pass through various pieces of PPE. Artificial blood is created to mimic real blood, including using thickening agents and red coloring to make it easier to spot. It's crucial to point out that this test is not rigorous, meaning that materials are not put under high-stress situations that may occur out in the field. Overall, this standard is designed to determine whether fluids such as blood can seep through the materials under normal circumstances.
- ASTM 1671 - Since PPE is supposed to prevent contamination of bloodborne pathogens, this test goes a step further than the one above by testing whether bacteria and other contaminants can penetrate the materials. In addition to having a visual examination with synthetic blood, the fluid contains Phi-X174 Bacteriophage, which acts as a suitable proxy for pathogens like HBV, HCV, and HIV.
When choosing personal protective equipment, it's crucial that each piece passes both of these standards. Any materials that are not rated for both of these tests will likely be insufficient at protecting workers and ensuring no cross-contamination.
Choose International Enviroguard for Your Bloodborne PPE Needs
Because healthcare workers are regularly exposed to various pathogens and hazardous materials, it's critical to have the right protective equipment in place. When choosing PPE, you want to make sure that it follows all CDC and OSHA guidelines, as well as ASTM tests.
ViroGuard® PPE is highly rated for many different applications, and we offer a wide array of protective options, including disposable coveralls, hoods, boot covers, and full body protective suits against blood and bloodborne pathogens. Even better, our PPE is designed for breathability and comfort without sacrificing any safety standards or procedures. Our materials have been put through rigorous testing to ensure that they can handle the many situations that can occur in the field. Some highlights of our PPE include:
- Thick materials with high abrasion resistance
- Taped seams for added protection from liquids seeping through exposed seams
- Large zippers make it easier to work with gloves
- Styles with built-in finger loops to prevent snagging and riding
- Styles with blue fabric to mask unsightly liquids and spills
- Bloodborne pathogen accessories such as hoods and boot covers for full body protection
ViroGuard®
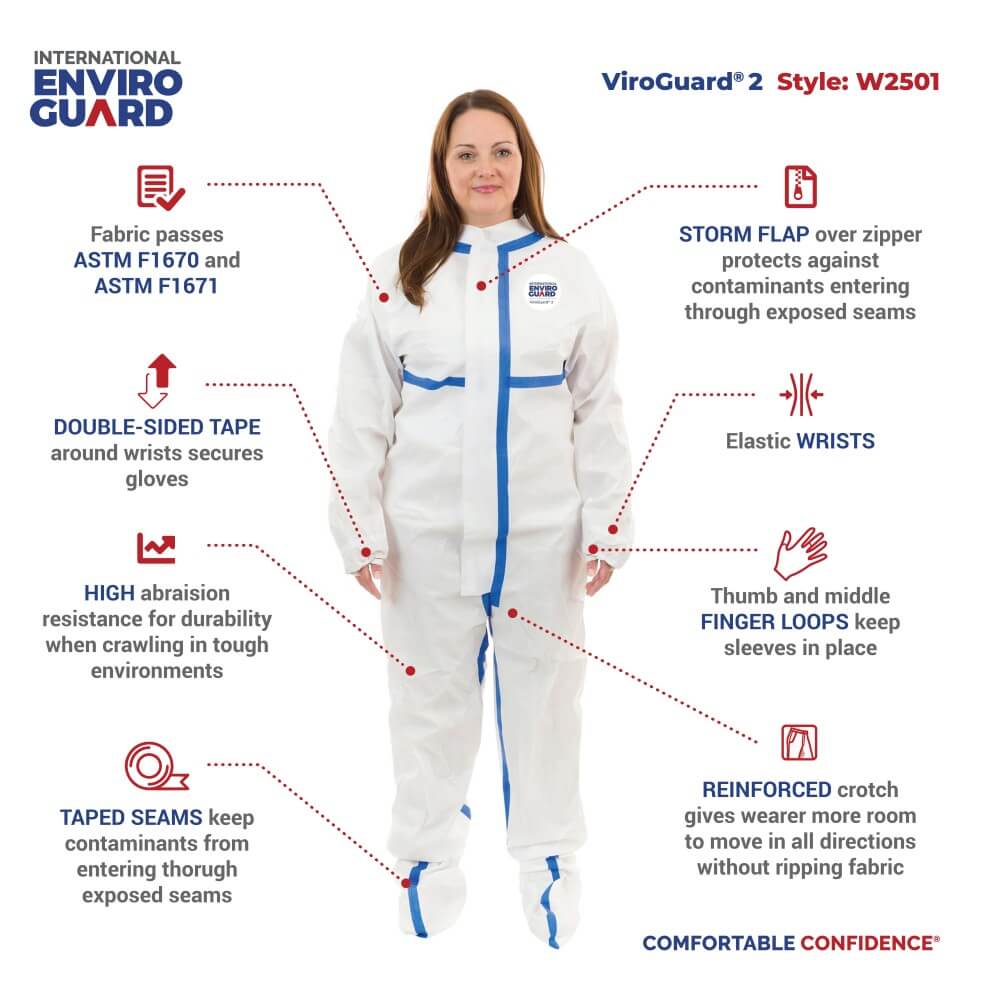
ViroGuard® 2
View all ViroGuard® PPE and accessories
Protecting your workers is a priority, and we make it easy to keep them safe. View our vast selection of healthcare PPE below: